A detailed, practical guide for people living with chronic kidney disease (CKD), their families, and advocates
1. Why Protein and Kidneys Are So Closely Linked
Your kidneys are your body’s filters. Every time you eat protein, your body breaks it down into building blocks (amino acids) and waste products (like urea and other nitrogen compounds). Healthy kidneys easily clear those wastes. When kidney function is reduced, that “waste removal” job becomes harder.
This is why:
- Too little protein → muscle loss, weakness, poor immunity, poor wound healing
- Too much protein → more waste for the kidneys to clear, which may speed up damage in some people with CKD
Key message:
Protein isn’t the enemy. The wrong amount and poor-quality sources can be a problem, especially as CKD progresses.
2. The Science of Protein and Kidney Health (Made Simple)
What protein does in your body
Protein is essential for:
- Maintaining muscle mass and strength
- Producing hormones, enzymes, and immune cells
- Healing from illness, surgery, or injury
- Maintaining skin, hair, nails, and organ function
Your body doesn’t have a big protein “storage tank” the way it stores fat. You need a steady, appropriate intake every day.
How kidneys handle protein waste
When you eat protein:
- Your digestive system breaks it into amino acids.
- Your body uses what it needs to build and repair tissues.
- The leftover nitrogen-containing parts are turned into urea, creatinine, and other waste.
- Your kidneys filter these wastes into urine.
With CKD, this process still happens—but more slowly and less efficiently. High protein intake means more waste, more filtration work, and higher pressure inside the kidney’s tiny filters (glomeruli).
Why high-protein diets can be risky in CKD
In people with existing CKD, consistently high protein intake can:
- Increase intraglomerular pressure (pressure within the kidney filters)
- Increase proteinuria (protein leaking into urine)
- Potentially accelerate decline in kidney function in susceptible individuals
Because of this, international guidelines now recommend avoiding high-protein diets (>1.3 g/kg/day) in people with CKD at risk of progression [KDIGO 2024]
3. How Much Protein Do You Actually Need? (By CKD Stage
Important: These are general ranges, not prescriptions. Your exact needs depend on weight, age, other conditions (diabetes, heart disease), and whether you’re losing protein in urine or on dialysis. Always confirm with your nephrologist and renal dietitian.
General protein ranges from guidelines
According to the 2024 KDIGO (Kidney Disease: Improving Global Outcomes) guidelines:
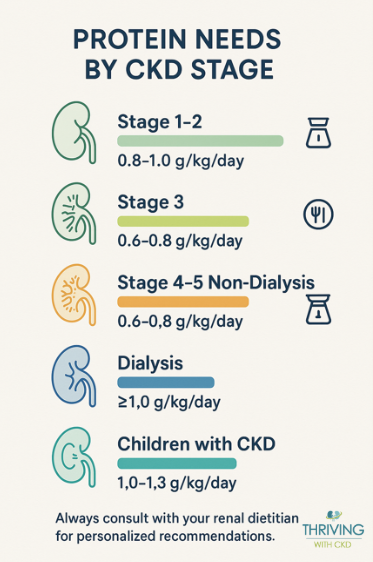
- Adults with CKD G3–G5 (non-dialysis):
Aim for around 0.8 g/kg/day of protein (similar to general population) and avoid going above 1.3 g/kg/day if you are at risk of progression [KDIGO 2024]. - Adults with CKD G4–G5 at high risk of kidney failure:
A low-protein diet around 0.6–0.8 g/kg/day can be considered. In very selected, closely monitored cases, a very-low-protein diet (0.3–0.4 g/kg/day) with keto acid analogs may be used, but only under specialist supervision and not in people who are metabolically unstable or malnourished [KDIGO 2024]. - People on dialysis (hemodialysis or peritoneal dialysis):
Dialysis removes amino acids and protein. Guidelines from KDOQI and other expert groups generally recommend higher protein intake, often 1.0–1.2 g/kg/day, to prevent malnutrition and muscle wasting (exact target from your dialysis team). - Children with CKD:
Do not protein restrict. Children need enough protein to grow; guidelines recommend intake toward the upper end of normal for age, not lower [KDIGO 2024].
What this looks like in real life (example)
For a 70 kg (154 lb) adult with CKD stage 3–4, non-dialysis:
- Target: ~0.6–0.8 g/kg/day
- That’s 42–56 g protein per day
Example daily pattern (~50 g):
- Breakfast: 2 scrambled eggs → ~12 g
- Lunch: 3 oz (85 g) grilled chicken → ~21 g
- Snack: ½ cup Greek yogurt → ~8–10 g
- Dinner: ½ cup cooked lentils → ~9 g
- Total: ~50–52 g
Individualization is critical
Across all stages, guidelines stress individualized assessment:
- Consider: CKD stage, weight, nutrition status, appetite, proteinuria, diabetes, phosphorus and potassium levels, and personal preferences.
- A renal dietitian is the best person to translate these targets into real meals you enjoy.
Key message:
Protein needs are individualized based on CKD stage and personal factors. “One-size-fits-all” plans from the internet can be harmful.
4. Plant Protein vs Animal Protein: What’s Better for Your Kidneys?
Big-picture differences
Animal proteins:
- Examples: Beef, pork, poultry, fish, eggs, dairy
- Tend to be complete proteins (contain all essential amino acids)
- Often higher in:
- Saturated fat (especially red and processed meats)
- Highly absorbable phosphorus
- Sodium and preservatives in processed meats (bacon, deli meats, sausages)
- Observational studies link high intakes of red and processed meat to higher risk of CKD and cardiovascular disease.
Plant proteins:
- Examples: Beans, lentils, chickpeas, soy foods (tofu, tempeh, edamame), nuts, seeds, whole grains
- Some are “incomplete” individually, but varied plant foods across the day provide all essential amino acids
- Typically:
- Lower in saturated fat
- Higher in fiber and phytonutrients
- Contain phosphorus that is less bioavailable (your body absorbs less of it) [University of Utah Health; National Kidney Foundation of Hawaii; CKDnutrition.com]
- Plant-based eating patterns have been associated with:
- Lower blood pressure
- Less metabolic acidosis
- Improved gut microbiome, fewer uremic toxins
- Slower CKD progression in some studies [Durham Nephrology; “Plant-Based versus Animal-Based Low Protein Diets in the Management of Chronic Kidney Disease,” PMC]
Why phosphorus matters in CKD
With reduced kidney function, phosphorus can build up and lead to:
- Itching, bone pain, and fractures
- Vascular calcification (hardening of arteries)
- Increased risk of heart disease
Key difference:
- Animal protein & additives → phosphorus is often highly absorbable (up to ~90%).
- Plant protein → phosphorus is often bound to phytate, and humans absorb much less (often ~30–50%), which can reduce phosphorus burden [CKDnutrition.com].
This is one major reason plant-forward protein choices are often preferred in CKD.
Best vs worst protein sources for kidney health
Below is a general guide. Your individual list may differ based on potassium, phosphorus, and sodium labs, plus other health issues.
Generally “better” protein choices (kidney-friendly patterns)
- Plant-based proteins (often preferred overall):
- Lentils, chickpeas, black beans, kidney beans (portion-controlled if potassium is high)
- Tofu, tempeh, edamame, soy milk
- Unsalted nuts and seeds (almonds, walnuts, chia, hemp, pumpkin seeds) – portion-controlled due to potassium/phosphorus
- Whole grains with modest protein: quinoa, farro, barley, oats
- Lean animal proteins:
- Skinless chicken breast or turkey
- White fish (cod, tilapia, haddock) and some fatty fish in moderation (salmon, trout) for omega‑3s
- Eggs or egg whites
- Plain Greek yogurt, cottage cheese (if phosphorus and potassium allow; choose lower-sodium versions)
- Features of “better” choices:
- Minimal processing
- Lower sodium and additives
- Lower saturated fat
- Lower phosphorus load or less absorbable phosphorus (plants)
Generally “worse” protein choices (limit or avoid in CKD)
- Processed meats:
- Bacon, sausage, hot dogs, deli meats, ham, pepperoni, salami
- High sodium, preservatives, often phosphate additives
- High-fat red meats:
- Fatty beef, lamb, ribs, burgers, organ meats
- High in saturated fat, and often significant phosphorus
- Foods with phosphate additives (check labels):
- Flavored meats, “enhanced” chicken/turkey, many fast foods
- Processed cheese products, cheese spreads
- Many packaged baked goods, colas, flavored drinks
- Look for ingredients containing “phos-” (e.g., sodium phosphate, phosphoric acid, pyrophosphate)
- Very large portions of animal protein at every meal
- E.g., a 12 oz steak in one sitting, or large double-meat sandwiches every day.
Key message:
Because plant-based proteins tend to produce less phosphorus burden and fewer uremic toxins, shifting toward more plant-dominant protein is often kidney-protective, especially in non-dialysis CKD.
Stage-Specific Protein Strategies
CKD Stages 1–2 (mildly reduced function)
Focus:
- Overall heart-healthy, kidney-protective eating pattern
- Avoid excess protein (especially bodybuilding-style high-protein diets)
Tips:
- Stay near 0.8–1.0 g/kg/day unless otherwise directed
- Emphasize plant-dominant proteins plus lean animal protein
- Limit processed meats and fast food
- Maintain healthy weight, blood pressure, and blood sugar
CKD Stage 3 (moderate reduction)
Focus:
- Slow progression, protect remaining function
- Avoid high-protein intake (>1.3 g/kg/day) [KDIGO 2024]
Tips:
- Aim around 0.8 g/kg/day unless dietitian advises otherwise
- Swap:
- Red/processed meat → beans, lentils, tofu, fish, poultry
- Large meat portions → moderate portions + plant protein side
- Start watching:
- Phosphorus and potassium if labs creeping up
- Sodium from processed meats and sauces
CKD Stage 4–5 (advanced, non-dialysis)
Focus:
- Carefully control protein load
- Prevent malnutrition while lowering kidney workload
Tips:
- Many people are advised toward 0.6–0.8 g/kg/day (individualized)
- Some may be candidates for very-low-protein diets with keto acid analogs under specialized, close supervision [KDIGO 2024]
- Partner very closely with a renal dietitian—this is not a do-it-yourself stage
- Pay attention to:
- High-phosphorus foods (especially with additives)
- High-potassium beans/lentils/soy if potassium is high (but small portions may still be allowed)
Dialysis (hemodialysis or peritoneal dialysis)
Focus:
- Prevent muscle wasting and malnutrition
- Replace protein lost during treatments
Tips:
- Typically need higher protein intake (often 1.0–1.2 g/kg/day or more) – confirm with your team
- Emphasize high-quality proteins at each meal and snack
- Still limit:
- Processed meats and phosphate additives
- Very high-phosphorus foods if labs are high
- Dialysis diet is complex (protein, fluid, potassium, phosphorus); professional guidance is essential.
6. Putting It Into Practice: Meal Planning Tips
Start with your target
- Get your protein target (g/day) from your nephrologist or renal dietitian.
- Divide by your usual number of meals/snacks.
- Example: 50 g/day with 3 meals + 1 snack → aim for ~12–15 g at each meal, ~8–10 g at snack.
Simple “plate planning” for CKD
A kidney-conscious plate often looks like:
- ¼ plate: Protein (plant or lean animal, portion sized to your target)
- ½ plate: Low-sodium, kidney-friendly vegetables and/or fruits (portion & type adjusted for potassium)
- ¼ plate: Kidney-friendly starch (rice, pasta, bread, tortillas, low-potassium grains)
Add:
- Healthy fats (olive oil, avocado in moderation, nuts/seeds if allowed)
- Plenty of herbs, spices, lemon, garlic, and vinegar instead of salty sauces
Practical swaps to improve protein quality
- Swap bacon/sausage → turkey slices, tofu scramble, or egg whites
- Swap double cheeseburger → grilled chicken or veggie burger on small bun
- Swap big steaks → 3–4 oz lean meat + side of lentils or quinoa
- Swap flavored yogurt (phosphate additives, sugar) → plain Greek yogurt with berries
Label-reading for kidney healthWhen choosing protein foods:
- Look at sodium: Aim for <140 mg/serving when possible (especially for regular items).
- Scan ingredient list for “phos-” words: If listed, phosphorus is added and highly absorbable—best to minimize.
- Compare plain versions vs flavored/marinated: Plain usually has less sodium and phosphorus.
Kidney-Friendly Recipe Ideas (Protein-Aware)
These are concept recipes to inspire you. Exact portion sizes and suitability depend on your stage, labs, and dietitian’s guidance.
Breakfast: Tofu & Veggie Scramble (Plant-Forward)Why it’s kidney-friendly:
Soft tofu provides high-quality plant protein with relatively lower phosphorus absorption than animal protein; vegetables add fiber and antioxidants with minimal sodium.
Ingredients (2 servings):
- ½ block firm tofu, drained and crumbled (~7–10 g protein/serving)
- ½ cup chopped bell peppers
- ½ cup chopped zucchini or mushrooms
- 1–2 Tbsp olive oil
- ¼ tsp turmeric, black pepper, garlic powder
- Salt-free seasoning blend (to taste)
Directions (concept):
- Sauté veggies in olive oil until softened.
- Add crumbled tofu and seasonings; cook until heated through and slightly browned.
- Serve with 1 small slice toast or ½ cup cooked rice (if appropriate for your carbs plan).
Adjustments:
- For higher protein (e.g., dialysis), add an egg or extra tofu.
- For potassium restriction, choose lower-potassium vegetables and keep portions small.
Lunch: Herb-Lemon Baked Chicken with Green Beans
Why it’s kidney-friendly:
Lean chicken offers controlled animal protein; cooking from scratch avoids phosphate additives and excess sodium.
Ingredients (2 servings):
- 6 oz (170 g) skinless chicken breast (3 oz per serving)
- 1 Tbsp olive oil
- 1–2 tsp dried herbs (thyme, oregano, basil)
- 1–2 cloves garlic, minced
- Juice of ½ lemon
- 1 cup fresh/frozen green beans
- Black pepper to taste
Directions (concept):
- Marinate chicken in olive oil, herbs, garlic, and lemon for 20–30 minutes.
- Bake at ~375°F (190°C) until cooked through (internal temp 165°F/74°C).
- Steam or sauté green beans with a bit of olive oil and garlic.
- Serve with ½ cup white rice or small baked potato (depending on potassium allowance).
Adjustments:
- CKD stages 3–4: Keep portion at ~3 oz cooked per meal.
- Dialysis: May increase portion size if higher protein needed per plan.
Dinner: Lentil & Vegetable Stew (Portion-Controlled)
Why it’s kidney-friendly:
Lentils are a nutrient-dense plant protein; when portion-controlled and tailored to potassium/phosphorus limits, they can be part of CKD diets, especially in earlier stages.
Ingredients (about 4 portions):
- 1 cup dry lentils, rinsed (use portion per dietitian guidance)
- 1 small onion, diced
- 1 carrot, diced (or use lower-potassium veg if needed)
- 1–2 stalks celery, diced
- 2 Tbsp olive oil
- 3–4 cups low-sodium vegetable broth or water
- 1 bay leaf, 1 tsp dried thyme, pepper
Directions (concept):
- Sauté onion, carrot, celery in olive oil until softened.
- Add lentils, broth, herbs; bring to a boil, then simmer until lentils are tender.
- Season with pepper and salt-free herbs; remove bay leaf.
Serving idea:
Serve a ½ cup portion of lentils as the protein component alongside a plate of non-starchy vegetables and rice/bread. Your dietitian may recommend smaller/larger portions based on potassium and protein targets.
Snack Ideas
Choose snacks that provide modest protein without excess phosphorus or sodium:
- ½ cup Greek yogurt (plain) with berries (if potassium allows)
- 1 small apple with 1 Tbsp almond or peanut butter (if potassium/phosphorus allow)
- ½ cup hummus (portion-controlled) with cucumber slices
- 1 boiled egg
- Unsalted popcorn + small handful (1 Tbsp) nuts
Key message:
Meal planning is about shaping your whole day’s intake—balancing total protein amount, source quality, and lab values—not perfection at every single meal.
8. Frequently Asked Questions from the Kidney Community
Q1: “My doctor told me to cut down on protein. Does that mean I should avoid it altogether?”
No. You still need protein every single day. The goal is not zero; it’s the right amount for your stage and individual situation. Too little protein can cause:
- Muscle loss and weakness
- Poor immunity
- Slower wound healing
- Increased frailty and falls
Work with a renal dietitian to set a specific daily target rather than just “cutting down.”
Q2: “Are high-protein diets (like keto or bodybuilding diets) safe if I have CKD?”
Most guidelines advise against high-protein diets (>1.3 g/kg/day) in people with CKD at risk of progression [KDIGO 2024]. These diets can:
- Increase kidney workload and intraglomerular pressure
- Increase urea and other waste products
- Potentially accelerate loss of kidney function in susceptible people
If you have CKD, you should not start a high-protein diet without discussing it with your nephrologist and dietitian.
Q3: “Everyone says plant protein is better. But can I still eat meat?”
In most cases, yes, you can still include some meat, especially lean, minimally processed forms. The general idea is to:
- Shift your pattern toward plant-dominant protein
- Choose lean poultry and fish more often than red/processed meats
- Keep portions moderate
- Combine smaller meat portions with plant proteins (e.g., chicken + lentils)
Your diet doesn’t have to be 100% vegan to gain benefits from more plant protein.
Q4: “Are beans, lentils, and nuts off-limits because of potassium and phosphorus?”
Not automatically. It depends on:
- Your current labs (potassium, phosphorus)
- Your portion sizes
- The rest of your day’s intake
Many renal dietitians are moving away from “banned” lists and instead using portion-controlled, plant-focused approaches. Small servings of beans, lentils, soy foods, and nuts may be allowed—even beneficial—if carefully planned within your overall limits.
Q5: “What about protein shakes or powders?”
Protein supplements can be tricky:
- Many are very high in protein (and often phosphorus, potassium, and additives).
- For non-dialysis CKD, they can easily push you above your recommended protein target.
- For dialysis patients with poor appetite, certain renal-formula supplements may be prescribed.
Always check with your nephrologist or dietitian before starting any protein shake or powder. If approved, they can help you choose lower-phosphorus, lower-potassium options.
Q6: “How do I know if my current protein intake is right?”
Look for these checkpoints:
- Lab values: stable or improving kidney function markers, phosphorus, potassium, albumin
- Body weight and muscle: stable weight (or intentional loss if overweight), no obvious muscle wasting
- Symptoms: adequate energy, fewer episodes of weakness or frequent infections
- Professional feedback: your care team is satisfied with your nutritional status
If you’re unsure, ask your provider for a referral to a renal dietitian to do a full nutrition assessment.
9. Partnering with a Renal Dietitian: Your Secret Weapon
Throughout all the major kidney guidelines (KDIGO, KDOQI, National Kidney Foundation), one message is repeated: nutrition therapy should be individualized and supervised by trained professionals.
A renal dietitian can help you:
- Translate grams of protein into real foods and recipes you enjoy
- Adjust protein intake over time as your CKD stage or dialysis status changes
- Balance protein needs with:
- Phosphorus limits
- Potassium limits
- Sodium and fluid recommendations
- Blood sugar control (if you have diabetes)
- Catch early signs of malnutrition or muscle loss and correct them
If you haven’t seen a renal dietitian yet, ask your nephrologist for a referral; in many countries, medical nutrition therapy is part of standard CKD care.
Key message:
You do not have to figure all of this out alone. Personalized guidance is part of good kidney care.
10. Key Takeaways
- Protein is essential. Your body needs it daily—but in CKD, the amount and source matter a lot.
- Avoid high-protein diets (>1.3 g/kg/day) if you have CKD at risk of progression, per KDIGO 2024.
- Typical targets:
- CKD G3–G5 (non-dialysis): ~0.8 g/kg/day, possibly 0.6–0.8 g/kg/day in advanced stages under supervision
- Dialysis: often 1.0–1.2 g/kg/day (or as advised)
- Children with CKD: do not restrict; they need enough protein to grow.
- Plant-forward patterns help:
- More beans, lentils, soy, nuts/seeds, and whole grains (within potassium/phosphorus limits)
- Less red and processed meat, fewer phosphate additives
- Quality over quantity:
- Lean, minimally processed proteins
- Limit processed meats and high-phosphate additives
- Work with a renal dietitian to tailor your plan to your labs, stage, medical history, and preferences.
- Protein isn’t the enemy. It’s about finding your sweet spot—enough to keep you strong and healthy, not so much that it overburdens your kidneys.
11. Cited & Referenced Resources
Clinical guidelines and major references:
- KDIGO 2024 Clinical Practice Guideline for the Evaluation and Management of Chronic Kidney Disease.
- Protein intake recommendations for adults with CKD G3–G5, guidance on high-protein diets, and very-low-protein diets with keto acid analogs.
- Kidney Disease: Improving Global Outcomes (KDIGO), 2024.
- KDOQI (Kidney Disease Outcomes Quality Initiative) Nutrition Guidelines.
- U.S.-focused guidance on protein needs in CKD and dialysis, including pediatric recommendations.
- National Kidney Foundation.
- “Plant-Based versus Animal-Based Low Protein Diets in the Management of Chronic Kidney Disease.”
- Peer-reviewed article discussing metabolic and clinical benefits of plant-based low-protein diets in CKD.
- Published in a nephrology journal via PubMed Central (PMC).
Patient-focused kidney nutrition resources:
- American Kidney Fund – Plant-Based Diets and Kidney Disease.
- Explains benefits of plant-based proteins vs red and processed meats for kidney health and cardiovascular risk.
- University of Utah Health – Kidney Disease and Phosphorus Education.
- Details on differences between plant and animal phosphorus absorption and why it matters in CKD.
- National Kidney Foundation of Hawaii – Plant-Based Protein and CKD.
- Educational materials on plant protein sources and phosphorus bioavailability.
- CKDnutrition.com – Phosphorus and Plant vs Animal Protein.
- Explains why plant-based proteins produce less phosphorus burden and fewer uremic toxins.
- Durham Nephrology Associates – Plant-Based Diets in CKD.
- Discusses potential benefits of plant-dominant diets on blood pressure, metabolic acidosis, and CKD progression.


